
סטיבן ראש, MD
פרופסור חבר לפסיכיאטריה קלינית ומדעי המוח ההתנהגותי
פסיכוזה משנית
חוויות פסיכוטיות שכיחות אצל אלו המאובחנים עם סכיזופרניה. למעשה, נוכחותם של תסמינים פסיכוטיים עלולה להוביל לאבחון של הפרעה מוחית זו אם הן אשליות והן הזיות קיימות במשך שישה חודשים, כולל חודש אחד של תסמינים מתמשכים. בהתמחויות רפואיות אחרות, אבחנה נעשית לעיתים קרובות לאחר בדיקה גופנית, הדמיה (צילומי רנטגן או CT) ובדיקות דם שהן חיוניות לקביעת אבחנה וטיפול מתאים. אולם בפסיכיאטריה, אותו תהליך אבחון אינו מניב לעתים קרובות מידע שימושי רב, למעט במקרה של פסיכוזה משנית (הנגרמת על ידי הפרעות רפואיות אחרות).
פסיכוזה משנית היא מונח שמשתמשים בו בתדירות גבוהה יותר בעשורים האחרונים, שכן ישנה הבנה הולכת וגוברת שחיוני להבין מתי תסמינים כגון אשליות והזיות נובעים ממחלה או חומר רפואי ידוע. בעבר כונו "פונקציונלי" כאשר יש לו מקור פסיכולוגי ו"אורגני" כאשר היה מקור ביולוגי ניתן לזיהוי, המעבר ל"ראשוני" ו"משני" משקף הבנה שלכל מצב פסיכיאטרי ותסמין יש מרכיב ביולוגי. הבנה זו הופיעה לראשונה בגרסה המתוקנת של המהדורה הרביעית של המדריך האבחוני והסטטיסטי להפרעות נפשיות (DSM-IV-TR) בשנת 2000. כל חומר, תרופה שנרשמה או מצב רפואי המשפיע על מערכת העצבים המרכזית עלול לגרום לתסמינים פסיכיאטריים כולל פסיכוזה, ולמרבה הצער, אנו ממשיכים לראות מקרים בהם אבחנה משוערת של סכיזופרניה נעשית לפני בדיקה רפואית יסודית הערכה מאשרת את היעדר מקור לפסיכוזה משנית.
במאמר משנת 2016 שפורסם ב-The Primary Care Companion to CNS Disorders, ד"ר João Gama Marques חקר באיזו תדירות לחולים שאובחנו בתחילה עם סכיזופרניה היה מקור בסיסי לפסיכוזה משנית שלא הוכר. ניתוח רטרוספקטיבי זה של 250 חולים בפורטוגל הראה של-25% מהחולים שאובחנו עם סכיזופרניה היו למעשה מצב רפואי בסיסי הגורם לתסמינים פסיכוטיים. ועוד, העיכוב הממוצע באבחון נכון היה 12 שנים. ההשלכות של עיכוב כזה באבחון יכולות להיות השלכות הרסניות לחולים ויקיריהם.
באמצעות מחקר של מדענים שנעשו במשך עשרות ומאות שנים אנו יכולים כעת לומר שפסיכוזה משנית יכולה לנבוע מ-13 קבוצות עיקריות של הפרעות שזוהו בגרפיקה הבאה.
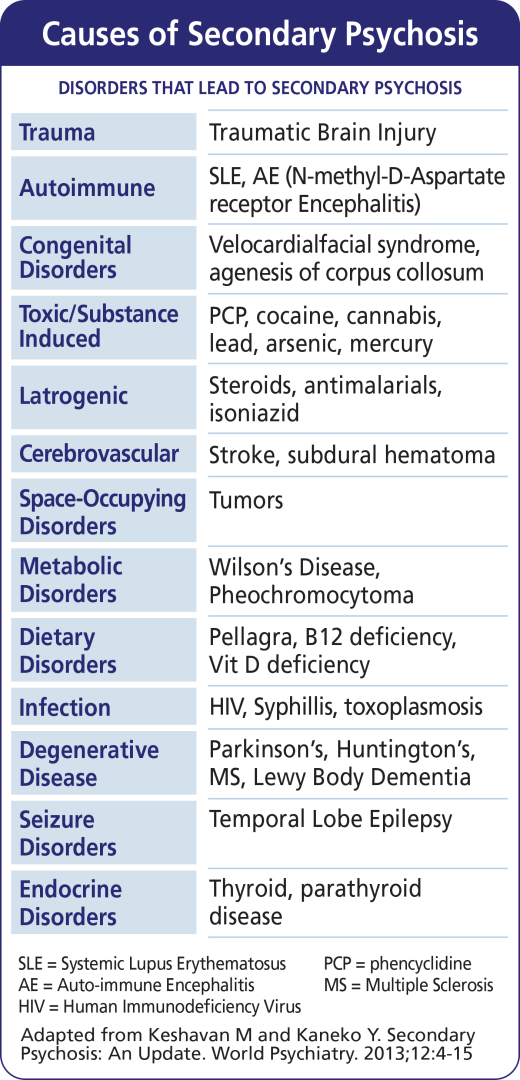
כיצד מטפלים קובעים אם הפרעה פסיכוטית היא "ראשונית" או "משנית"? ראשית, יש לזהות את החומר הסיבתי או את המצב הרפואי. לאחר מכן, יש לזהות את הקשר בין מצב רפואי או חומר בשימוש לבין התסמינים הפסיכוטיים. בתוך כך, על הרופאים לשקול שלושה היבטים מרכזיים של הסימפטומים של המטופל: לא טיפוסיות, זמניות והסבריות.
יש לחשוד בגורם רפואי בסיסי לפסיכוזה אם המצג הוא לֹא טִיפּוּסִי ביחס לגיל ההופעה וסוג התסמינים שנצפו. לדוגמה, נוכחותם של מספר סוגים של הזיות (שמיעתית, חזותית, מישוש וחוש הריח) אינה אופיינית בסכיזופרניה ומגבירה את הסבירות להפרעה פסיכוטית משנית כמו אלו הנראות בדמנציה או סוגים מסוימים של אפילפסיה. ה זמניות של התסמינים, או כאשר הם מתרחשים, יש לשקול כאשר התסמינים הפסיכוטיים מגיעים לאחר תחילתה של מחלה רפואית או בליעה של חומר וחולפים כאשר המצב הרפואי משתפר, או שהחומר מסולק מהגוף. לבסוף, מכיוון שמחלות רפואיות נלוות שכיחות מאוד אצל אנשים הסובלים מסכיזופרניה, חשוב לשאול אם התסמינים הקיימים הם הטובים ביותר הסביר על ידי הפרעה פסיכוטית ראשונית או משנית. לדוגמה, בחולה עם היסטוריה משפחתית חזקה של סכיזופרניה אצל הוריו ואחיו, תסמינים פסיכוטיים ארוכי שנים, אפילו בהקשר של מחלה רפואית מתרחשת במקביל, עשויים להיות מוסברים בצורה המדויקת ביותר על ידי סכיזופרניה בהינתן הנטייה הגנטית הקיימת.
באפריל 2018, המרכז הרפואי של אוניברסיטת סינסינטי הנהיג את תוכנית ההערכה והשירותים של פרק ראשון (FEELs). זה כולל צוות רב תחומי של רופאים, אחיות, עובדים סוציאליים, רוקחים, פסיכולוגים, מרפאים בעיסוק ופנאי הפועלים יחד כדי לשלול גורמים משניים לפסיכוזה בחולים בשנתיים הראשונות להופעת התסמינים כשהם ביחידה אשפוזית פסיכיאטרית. בדיקה זו כוללת בדיקות דם יסודיות, הדמיה, סקירה של כל התרופות שנלקחו וחומרים ובדיקות פסיכולוגיות. הערכה זו מסייעת לצוות המטפל לזהות את הגורם הסביר ביותר לפסיכוזה בכל מטופל נתון ולהנחות את הטיפול. אם מזוהה מצב רפואי, קלינאים המתמחים בטיפול במצב זה מעורבים בטיפול. פרוטוקול זה נוצר בהשראת עבודה עם חולים שהפרעות פסיכוטיות משניות לא זוהו בשלב מוקדם של מחלתם, מה שהוביל להשלכות שליליות ארוכות טווח. בעוד שבמרכזים רפואיים אקדמיים רבים יש נהלים דומים, עדיין יש חוסר מודעות לגבי הגורמים הניתנים לזיהוי של פסיכוזה משנית במקומות רבים ברחבי העולם. רופאים, מטופלים ובני משפחה כאחד חייבים לקבל השכלה לגבי נושאים אלה ולתמוך בהערכה סטנדרטית של גורמים משניים לפסיכוזה כדי לקדם את המטרה המשותפת שלנו של ריפוי באמצעות אבחון וטיפול נכונים.
הפניות:
Keshavan MS, Kaneko Y. פסיכוזות משניות: עדכון. פסיכיאטריה עולמית. 2013;12(1):4-15. doi:10.1002/wps.20001
Gama Marques J. פסיכוזה אורגנית הגורמת לסכיזופרניה משנית ברבע מקבוצה של 200 חולים שאובחנו בעבר עם סכיזופרניה ראשונית. מִצטַנֵעַ
טיפול מלווה בהפרעה במערכת העצבים המרכזית. 2020;22(2):19m02549.

